Child
- About
- Meet The Team
- Conditions
- Dental Practitioners: Dental care in children at risk of Infective Endocarditis
- Looking after your child’s oral health
- Coming for an echocardiogram
- Outpatient Appointments
- Preparing to Come into Hospital for Surgery
- On Admission to the Children's Ward
- Visiting
- Operation Day
- Children's Intensive Care
- Daily Routine on Intensive Care
- Managing your child's discomfort
- Going Home
- Children's Cardiac MRI Scan
- Cardiac Catheter
- Reveal Device
- Ablation Procedure
- Pacemakers
- INR and Warfarin
- Lifestyle and Exercise Advice
- School Advice
- Attachment
- Yorkshire Regional Genetic Service
- Advice & Support Groups
- Your Views
- Monitoring of Results
- Second Opinion
Children's Intensive Care
-
Welcome to Ward L47, the Children’s Cardiac and General Intensive Care unit at Leeds General Infirmary.
Having a child in intensive care can be very stressful and worrying time for you as parents. The aim of these pages is to explain how the unit works and some of the language used. The information here is designed to help you during your stay. It has practical advice about what to expect and we hope it will help you feel less anxious when visiting your child.
-

-
Ward L47 has up to 18 beds consisting of 10 cubicles and a big 8 bed bay area. A sitting room is provided for parents, which has a payphone, television and drink making facilities. There is also a visitor’s toilet. Your nurse will be happy to show you these facilities.
Most children are admitted to the unit from theatre after being on the children’s ward. However, some are admitted directly from another hospital. All of these children are nursed on the unit because they are very poorly and need specialised nursing and medical care.
-
Common Equipment on PICU
Your child may need many types of equipment to enable the doctors and nursing staff to monitor your child very closely and to administer prescribed medications. The following list aims to introduce you to most of the equipment used. The nurse caring for your child will be very happy to explain the need for and function of any equipment in use.
Arterial Line
This is a special line going into an artery. This is connected to the monitor and measures the blood pressure. It can also be used by the nurses to take blood samples.
Chest Drain
These are drainage tubes, which come out of the chest and are connected to containers under the bed. These drain excess blood from the operation site and allow for the lungs to re-expand fully.
-
Drugs and Medicines
Your child will be given many drugs. These include strong painkillers and antibiotics. Some drugs are used to support the heart during recovery.
Endotracheal Tube
This breathing tube goes from the nose (or sometimes the mouth) into the lungs. It is attached to the ventilator. The tube passes through the vocal cords so your child won’t be able to cry or speak. The tube is taped in securely to prevent it from becoming dislodged. To prevent this tube from becoming blocked a thin tube is used to suck up secretions. This is called suctioning. This may make your child cough. Some parents find this upsetting.
-
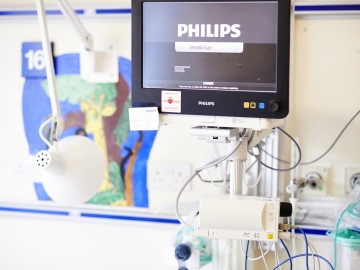
Monitor
Each space has a main monitor (television screen) to measure heart rate, blood pressure and other things. All of the equipment has alarms. These are very sensitive and sometimes go off when nothing serious is wrong. The nurse looking after your child will check if an alarm goes off.
Intravenous Lines
Your child will have 1 or 2 intravenous lines in their neck/leg to enable us to give drugs and fluids. These lines may be attached to syringe pumps or infusion pumps, which allow the exact amount of fluid to be infused.
-
Nasogastric Tube
This tube goes from the nose into the stomach. This allows us to aspirate his/hers natural gastric juices and air so that he/she does not vomit. Later the same tube may be used for feeding purposes.
-
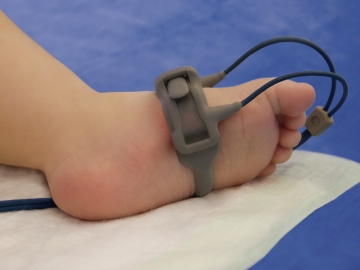
Oxygen Saturation
This is attached to a finger or toe to measure the oxygen in the blood.
Pacing Wires
These thin wires come out through the chest to be attached to a pacemaker box. These can be used to make the heart beat faster. The pacemaker is not always used.
Peritoneal Dialysis Catheter
This is another drainage tube which may be used to support your child’s kidneys if they do not work adequately.
-
Temperature probes
There will be a small probe inserted into your child’s bottom or nose to measure central temperature and another probe attached to the foot to measure skin temperature. This gives an indication of how well the heart is functioning.
Urinary Catheter
This tube goes into the bladder. We measure the amount of urine hourly. This gives us an indication of how well the kidneys are functioning and whether the heart is pumping enough blood to allow this.
Ventilator
This machine takes over your child’s breathing until they are able to breathe for themselves. Your child will not be able to eat or drink whilst attached to the ventilator; however we will provide nutrition via different routes such as a drip or nasogastric tube.
