Teen
- About
- Meet The Team
- Conditions
- Aortic Stenosis
- Atrial Septal Defect
- Coarctation of the Aorta
- Complete Atrioventricular Septal Defect
- Interrupted Aortic Arch
- Normal Heart
- Partial Atrio-Ventricular Septal Defect
- Patent Ductus Arteriosus
- Pulmonary Atresia with Intact Ventricular Septum
- Pulmonary Atresia with Ventricular Septal Defect
- Pulmonary Stenosis
- Small Ventricular Septal Defect (Muscular)
- Small Ventricular Septal Defect (Perimembraneous)
- Tetralogy of Fallot
- Transposition of the Great Arteries
- Ventricular Septal Defect (Large)
- Transition to Adult Congenital Cardiac Services
- Coming in to Hospital
- Surgery and Managing Your Discomfort
- Cardiac Catheter
- Ablation Procedure
- Pacemakers
- Looking after your oral health
- Lifestyle and Exercise Advice
- Periods, contraception and pregnancy
- Support
- Your Views
- Confidentiality and Consent
Interrupted Aortic Arch
This is a very serious heart condition in which there is a complete blockage in the main artery (the aorta) which comes off the heart to feed the body with blood. The blockage usually occurs just after the aorta has given off branches to supply the head and arms with blood, preventing normal circulation to the lower half of the body.
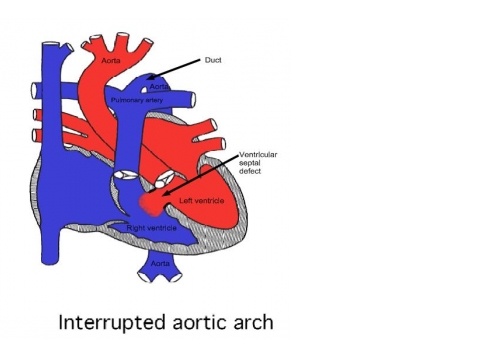
Babies with this abnormality also have a hole between the two main pumping chambers of the heart (a ventricular septal defect, or VSD).
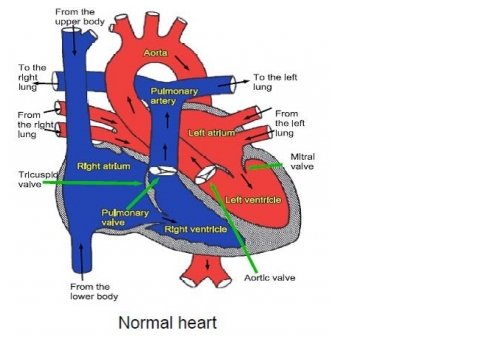
Before birth the two main arteries coming off the heart (one leading to the lungs, the pulmonary artery and one leading to the body, the aorta) are joined together by a short blood vessel called the arterial duct. The duct allows blood to get to the lower half of the body from the pulmonary artery. For this reason most babies with interrupted aortic arch are well before birth and appear perfectly well immediately after birth.
However, the duct is designed to close itself off (it has muscles in its wall) within the first week or so after birth because it is no longer required in the normal circulation.
When this happens in a baby with an interrupted aortic arch the baby becomes extremely ill because no blood reaches the lower half of the body, making it difficult for the heart to pump normally and the baby will die without treatment.
Tests
Usually only simple tests such as an ultrasound scan of the heart (an “echo”), and an x-ray of the chest are required
Treatment
Surgery is necessary to repair the aorta and to close the VSD, but before this is carried out it is important to get the baby as well as possible if the baby is to survive. First of all a medicine called prostin is given as a continuous injection into one of the baby‘s veins. Prostin relaxes the muscles in the wall of the duct, allowing it to open up so that blood can flow again to the lower half of the body. Sometimes we will delay surgery for several days to get the baby as well as possible.
Risks of treatment
Most babies with interruption of the aorta will survive surgery and go on to lead normal lives, but there is a small risk (about 2 in 100) of the baby dying at or shortly after the operation. Complications such as pneumonia, other infections or kidney damage can occur but most babies recover from these. There is also a small risk (about 1 in 100) of major complications such as brain damage or damage to the spinal cord which carries the nerves to the lower half of the body.
Spinal cord damage is a very serious complication as it does not usually recover and the baby is left with permanent paralysis.
Follow up after operation
Sometimes as the baby grows the repair of the aorta does not, and this can lead to narrowing in the aorta which may require further treatment. It is also common to develop new narrowing in the outlet of the left ventricle (just below the outlet valve or at the outlet valve itself), even after initial surgery. If these narrowings develop they can be serious and may require further major surgery or even valve replacement as the child grows. Even many years after operation it is possible to develop a weak spot (called an aneurysm) in the wall of the aorta, which can also require further surgery. Regular checkups in the outpatient clinic are therefore necessary throughout the patient’s life.
Other abnormalities
Some children with interruption of the aortic arch have other abnormalities. The commonest of these is a genetic abnormality, where a small part of one chromosome is missing. This abnormality is called “22q11 deletion” and is sometimes referred to as “DiGeorge Syndrome”. Although some children with 22q11 deletion grow and develop normally, some will have learning or speech difficulties or difficulty fighting certain types of infection. If your baby has 22q11 deletion it is important that his or her development is monitored so that help can be given early if necessary. A blood test to check for this abnormality is usually done, but it may take some weeks for the result to come back.
Endocarditis
There is a small risk of infection occurring in the aorta or on one of the heart valves (called endocarditis). This can happen even years after the operation and can be caused by infection of the teeth or gums. It is very important to visit the dentist regularly and to remind the dentist at each visit of the heart abnormality. Infection occurring with ear and body piercing and tattooing can sometimes also lead to endocarditis, so these procedures are best avoided.
